You need sleep to keep your brain functioning and your memory sharp. So, it’s not completely surprising that poor sleep is a potential risk factor for Alzheimer’s disease.
The most common form of dementia, Alzheimer’s is a brain disorder that progressively destroys someone’s memory and thinking skills. The lack of restorative sleep can damage areas throughout the brain.
Here’s how sleep can affect your risk of Alzheimer’s disease and dementia.
How Does Sleep Impact Your Risk of Developing Alzheimer’s?
Poor sleep quality can change the brain, potentially contributing to development of Alzheimer’s disease or other forms of dementia. Research doesn’t fully explain the link, but it appears that poor sleep may lead to brain changes that eventually lead to Alzheimer’s disease. Additionally, Alzheimer’s is also known to disturb sleep.
The Link Between Sleep and Alzheimer’s Disease
Alzheimer’s usually affects people 65 years of age or older. As you age, you’re also more likely to have trouble sleeping. In a study including people aged 65 and older, those who slept less than five hours doubled their risk of developing dementia compared to those sleeping six to eight hours. Another study in people aged 50-70 found that sleeping six or fewer hours increased dementia risk by 30% compared to those sleeping for seven hours.

“Poor sleep is increasingly recognized as a potential risk factor for Alzheimer’s disease,” says Dr. Rizwan Bashir, a board-certified neurologist at AICA Orthopedics in Atlanta. “Research suggests that disrupted sleep patterns can interfere with the brain’s ability to clear out amyloid-beta, a protein that accumulates abnormally in the brains of those with Alzheimer’s. Consistently poor sleep may, therefore, contribute to the development and progression of the disease.”
Studies show that poor sleep quality, difficulty falling asleep, excessive daytime sleepiness, and sleep-disordered breathing are all associated with an increase in amyloid-beta proteins in older adults without dementia. When these proteins accumulate in the brain, they trigger inflammation and death of neurons—a type of brain cell that helps send messages to your body to breathe, talk, walk, and think. This effect impairs cognitive functions such as memory and reasoning. As more amyloid-proteins accumulate, cognitive function continues to decline.
“The connection between sleep and Alzheimer’s disease might involve several neurological pathways, most notably through the glymphatic system, which is active during sleep,” says Bashir. “This system helps to clear out waste from the brain, including the aforementioned amyloid-beta proteins.”
Sleep Disorders that May Be Associated with Dementia
It is common for people with dementia to develop sleep disorders. Researchers estimate 25% of adults with dementia also have a sleep disorder. Sleep disorders often appear before an Alzheimer’s diagnosis, and these disorders get worse as the condition progresses. However, it’s not fully understood if the cognitive decline of dementia leads to sleep disorders or if sleep disorders lead to dementia.
Insomnia
Insomnia is a sleep disorder where it is difficult to fall asleep, stay asleep, or get good quality sleep. This is the most prevalent sleep disorder among adults. Insomnia leads to daytime sleepiness and sleep deprivation. It can also affect your memory and concentration.
Research shows sleep deprivation and insomnia can cause the brain to accumulate Aβ peptides and tau proteins, which leads to Alzheimer’s disease. Research has shown that sleep-initiation insomnia, meaning difficulty falling asleep, may increase the risk of developing dementia. Chronic insomnia—which occurs three or more times weekly for three months—also increases your risk of Alzheimer’s risk factors like high blood pressure and diabetes.
Sleep Apnea
Sleep apnea is a condition that causes someone to stop breathing in their sleep. This can lead to gasping for air, poor sleep, and a lack of oxygen to the brain (hypoxia). Obstructive sleep apnea (OSA) happens when the upper airway is physically blocked during sleep, cutting off airflow. Central sleep apnea occurs when the brain doesn’t send signals to the body to breathe.
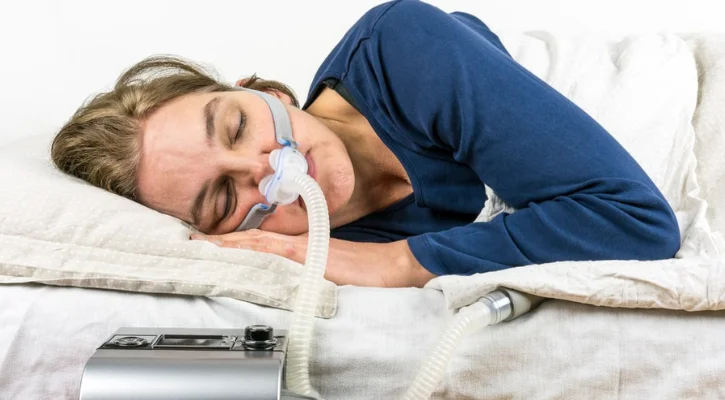
People with sleep apnea are at an increased risk of developing dementia like Alzheimer’s disease. Studies show people with OSA may lead to poor cognitive functions like memory consolidation. Lack of oxygen and OSA also appear to increase the accumulation of amyloid-beta peptides in the brain, a biomarker of Alzheimer’s. However, people with Alzheimer’s are also at an increased risk of developing OSA after their diagnosis.
Restless legs syndrome
Restless legs syndrome (RLS) is a neurological sleep disorder that causes involuntary leg movements or sensations at night. People with the condition are prone to dementia risk factors like poor sleep quality and hypoxia.
It’s not fully understood if RLS itself or the increase in sleep disturbances—like falling asleep and getting enough sleep—leads to dementia. However, people with RLS often have an increase in Alzheimer’s brain plaques caused by reduced slow-wave sleep and extremely poor sleep. Studies have also shown that people with RLS have decreased gray and white matter volume in their brains, which are signs of neurodegeneration.
REM Sleep Behavior Disorder
During the REM (rapid eye movement) sleep stage, the body is temporarily paralyzed, the eyes rapidly move, and dreaming occurs. People with REM sleep behavior disorder (RBD) have periods where temporary muscle paralysis stops, and they physically reenact dreams during their sleep. This often leads to poor sleep and people injuring themselves or their partners during vivid dream episodes.
Research has found 30% of people with RBD develop Parkinson’s disease or dementia with Lewy bodies in three years. That increased to 66% in seven and a half years. Dementia with Lewy bodies is associated with abnormal alpha-synuclein proteins in the brain that lead to problems thinking, moving, and regulating mood. People with RBD also appear to start accumulating more alpha-synuclein proteins in the brain that cause dementia.
Research-Backed Ways to Reduce Your Risk of Alzheimer’s
In addition to poor sleep quality, Alzheimer’s risk factors for adults 45 and older include high blood pressure, physical inactivity, obesity, diabetes, depression, smoking, and binge drinking.
“While there is no guaranteed way to prevent Alzheimer’s, research supports several strategies that may reduce risk,” notes Bashir. Some proven ways to reduce these Alzheimer’s risk factors include:
- Limit processed foods and eat nutritious foods like fruits, vegetables, proteins, and whole grains.
- Stay physically active with at least 150 minutes of moderate-intensity physical activity and two days of strength training each week.
- Quit smoking and limit alcohol to a moderate amount (two drinks daily for men or one drink for women).
- Improve your sleep by setting up a routine bedtime and wake up time, avoiding screen time and caffeine before bed, and sleeping for at least seven hours nightly.
FAQs about Sleep and Alzheimer’s
Is sleep a risk factor for Alzheimer’s?
Poor sleep is considered a risk factor for developing Alzheimer’s disease and other dementias. Research shows people often experience sleep disruption years before developing Alzheimer’s symptoms. Other research shows just losing 1% of deep sleep yearly increases dementia risk by 27%. People who have trouble falling asleep also appear to have an elevated dementia risk.
How many hours of sleep do you need to prevent Alzheimer’s?
Sleeping six to eight hours every night may help prevent Alzheimer’s disease. Research suggests that getting six hours of sleep or less in your 50s and 60s increases the risk of developing Alzheimer’s disease and other dementias.
What is the most common bedtime habit that triggers dementia?
Sleep habits like an early bedtime and taking sleep medications may increase your risk of developing dementia. A Chinese study of people aged 60-74 found those who went to bed before 9 p.m. were at an increased risk of Alzheimer’s disease. People who use sleep medications to fall asleep also appear to have an elevated dementia risk.
Bottom Line
It’s not clear whether sleep problems are a very early sign of predisposition to dementia, or whether lack of sleep causes dementia. Researchers of a small 2017 study found that treating sleep disorders resulted in more deep sleep and better clearance of beta amyloid from the brain (a cause of Alzheimer’s disease). So, even if you are not getting a good night’s sleep, you can reduce your likelihood of dementia by making your sleep environment more comfortable and integrating relaxation, meditation, and stress relief into your life.


